What is Depression?
Depression is more than just a temporary "bout of the blues." It is a clinical syndrome that impairs your ability to function at work, school, and home. To be diagnosed with Major Depressive Disorder, symptoms must be present for at least two weeks and represent a change from your previous level of functioning.
While MDD is the most common form, several other types exist:
-
Persistent Depressive Disorder (Dysthymia): A longer-lasting, less severe form of depression that continues for at least two years.
-
Anxious Depression: Depression accompanied by high levels of tension and restlessness; this is currently the most common presentation.
-
Seasonal Affective Disorder (SAD): Depression that correlates with the change in seasons, typically beginning in the autumn.
-
Peripartum Depression: Depression occurring during pregnancy or after childbirth.
Causes of Depression
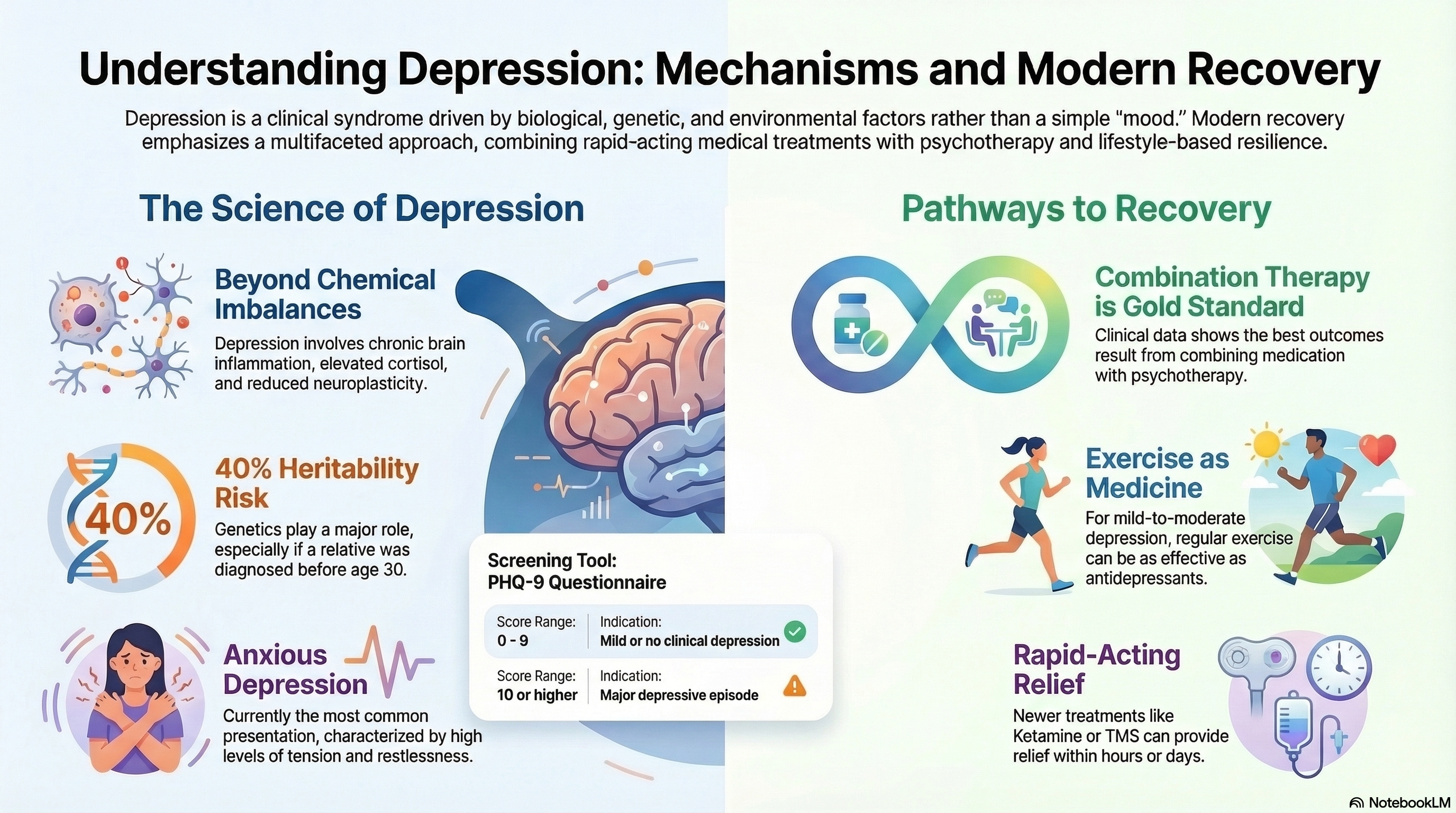
Modern medicine recognizes that depression is not caused by a single factor, but rather a combination of biological, genetic, and environmental triggers.
-
Biological Mechanisms: Research has moved beyond the "chemical imbalance" theory. We now know depression involves chronic low-grade brain inflammation, elevated stress hormones (cortisol), and reduced "neuroplasticity" (the brain's ability to repair and reorganize itself).
-
Genetics: Depression has approximately 40% heritability. If a close relative has had depression, especially before age 30, your risk is higher.
-
Brain Chemistry: Neurotransmitters like serotonin and dopamine play a role, but newer research highlights glutamate—which is why rapid-acting treatments like ketamine are becoming more common.
-
Life Events: Childhood trauma, chronic stress, or the loss of a loved one can trigger biological changes that lead to depression.
-
Medical Conditions: Chronic pain, strokes, heart attacks, and thyroid disorders are frequently linked to depressive episodes.
Symptoms of Depression
Depression manifests differently in everyone. While some feel overwhelming sadness, others may primarily experience physical pain or extreme fatigue.
Core Symptoms:
-
Depressed mood (feeling sad, empty, or tearful) nearly every day.
-
Loss of interest or pleasure in almost all activities (anhedonia).
-
Significant changes in appetite or weight.
-
Sleep disturbances (insomnia or sleeping too much).
-
Fatigue or loss of energy.
Cognitive and Physical Symptoms:
-
Brain Fog: Difficulty thinking, concentrating, or making simple decisions.
-
Feelings of Worthlessness: Excessive or inappropriate guilt.
-
Physical Aches: Unexplained headaches, back pain, or digestive issues.
-
Irritability: "Rage attacks" or persistent frustration, which is particularly common in men and adolescents.
Diagnosis of Depression
There is no blood test for depression; it is a clinical diagnosis based on a thorough evaluation by a healthcare provider.
-
Clinical Interview: A doctor or therapist will discuss your history and the duration of your symptoms.
-
Screening Tools: The Patient Health Questionnaire-9 (PHQ-9) is a widely used 9-question tool. A score of 10 or higher typically indicates a major depressive episode.
-
Physical Exam: Your doctor may order blood work to rule out other medical causes, such as vitamin B12 deficiency or hypothyroidism, which can mimic depression.
-
Somatic Probing: Because many patients first report "tiredness" or "pain" rather than sadness, doctors are trained to look for depression behind these physical complaints.
Treatment of Depression
Depression is one of the most treatable mental health conditions. In 2026, the range of options is broader and more effective than ever before.
-
Psychotherapy: "Talk therapy" is highly effective. Cognitive Behavioral Therapy (CBT) helps change negative thought patterns, while Behavioral Activation focuses on re-engaging with positive activities.
-
Medications: * SSRIs and SNRIs: Common first-line treatments like sertraline or venlafaxine.
-
Atypical Antidepressants: Options like Bupropion (for low energy) or Mirtazapine (for insomnia).
-
-
Rapid-Acting Treatments: For severe or treatment-resistant cases, Esketamine nasal spray or IV Ketamine can provide relief within hours or days rather than weeks.
-
Brain Stimulation: Transcranial Magnetic Stimulation (TMS) uses magnetic fields to stimulate nerve cells in the brain and is non-invasive.
-
Combination Therapy: Data shows that the best outcomes generally result from combining medication with psychotherapy.
Prevention of Depression
While you cannot always prevent the onset of a biological illness, you can build "psychological resilience" and maintain brain health.
-
Exercise: For mild-to-moderate depression, regular exercise is proven to be as effective as antidepressants. Aim for 30 minutes of moderate activity 3–5 times a week.
-
Sleep Hygiene: Prioritizing consistent sleep cycles helps regulate the brain's stress response.
-
Dietary Choices: An anti-inflammatory or Mediterranean diet (rich in Omega-3s) supports brain health.
-
Stress Management: Mindfulness-based practices can help prevent the "relapse" of symptoms after you have recovered.
-
Limit Substances: Reducing alcohol and cannabis use is vital, as both are depressants that can worsen the long-term course of the illness.
If you or someone you know is in crisis, immediate help is available. In the US and Canada, you can call or text 988. In the UK, call 111 or 116 123.




